Over the last decade, many of the mysteries regarding the role of microbes in human health have been solved. No longer are these invisible organisms solely regarded as pathogens. They represent a diverse community of species, most of which are harmless and others actually help us stay healthy. But there is one particular enigma for which there appears to be no answers. It's known as the "hygiene hypothesis" and is best described by a relatively simple question:
Are we too clean?
The theory was first developed back in 1989 when researchers noticed a higher level of hay fever in children. The cause for this appeared to be a lack of exposure to respiratory viruses and subsequent infection in early childhood. Although this seemed odd at first, from an immunological perspective, it made sense.
When a person becomes infected with a virus, the immune system fights back to get rid of the invader. During the battle, some of the cells responsible for the defence memorize the molecular makeup of the pathogen. This memory ensures a quick and effective response should there ever be another incursion. This memory is best developed during childhood.
If, however, the virus is first introduced later in life, the immune system may not know how to act properly. Instead of carrying an all-out anti-viral attack, some children may experience an allergic response. Unfortunately, this also leads to memory meaning any further exposure to these viruses would end up in an allergic attack.
The idea of infecting young children in order to prevent allergies later in life may not be a standard practice for most parents. Children have enough troubles in those early years without the addition of infections. Besides, the initial theory was based on head counts rather than an actual mechanism. It's why over the years the hypothesis has been examined and re-examined in order to figure out whether it was correct.
Most of the work focused on the immune system in the hopes of better understanding memory. There was little gained in terms of answering the question. But in 2009, a new direction suggested the focus on immunity was perhaps misplaced. Instead of worrying about infection and immunity, researchers should have focused on the presence and lack of a group of microbes known simply as Old Friends.
In essence, allergies were not a result of a lack of pathogen exposure but instead a lack of Old Friends.
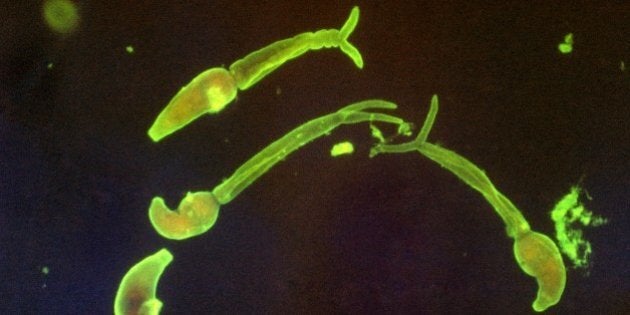
The change was due to a rather odd remedy for allergies. Instead of drugs, some researchers found they could use microbes -- in this case, worms. Officially known as helminths, these microscopic wrigglers could be used to treat certain allergies. When researchers took a closer look at how these supposed pathogens were actually helping people, they found a surprising result. These organisms were somehow working to balance the immune system so that it would not overreact and lead to allergies.
But worms were not alone in their ability to balance immunity. Other microbes, such as probiotics and several environmental species, also had the ability to carry out the same balancing act. This prompted examinations of the microbial population of individuals to determine if there were any trends in those with allergies.
Sure enough, there was one specific trait common to those who suffer. They all had a lower diversity of microbes and for the most part were missing a number of species known to be friendly to us. In essence, allergies were not a result of a lack of pathogen exposure but instead a lack of Old Friends.
As result of the compilation of studies, a group of hygiene researchers wondered whether the end was near for the hygiene hypothesis. Last week, they published an examination of the perceptions of experts to determine whether they agreed the time had come to move on. The results revealed there was more than enough evidence to put the nearly 30-year old theory to bed.
Though this may signal the end of the hygiene hypothesis, there is still a need to explain the formation of allergies in children. For the researchers, the answer comes down to a lack of Old Friends. In absence of these microbes, the immune system loses its ability to stay balanced and can overreact when infection occurs. To prevent this occurrence, friendly species need to be fostered and fed through a combination of exposure to a diverse environment as well as a friendly diet, which for babies, includes breast milk.
As for hygiene, the researchers suggest there is even more reason to be hygienic in the home and elsewhere. Without the need for exposure to infections, the acts of cleaning, disinfecting and keeping those hands clean is more important than ever.
Besides, getting closer to those Old Friends won't happen through exposure in the home, school or office. The best way to do this is to get outside and explore a variety of different areas such as parks, forests and farms. In addition, ensure the diet is rich in foods promoting these friendly species including polyunsaturated fats, fibre and fermented foods.
Follow HuffPost Canada Blogs on Facebook
MORE ON HUFFPOST:
