
Ovarian cancer doesn't have the high public profile of breast cancer, or the simple testing option of cervical cancer, but it's the most serious women's cancer in Canada — and the fifth most common cancer in women overall.
An estimated 2,800 Canadian women will be diagnosed with ovarian cancer this year, according to Ovarian Cancer Canada, and 1,800 will die of the disease. But because it's not as well known by the general public, and because its symptoms are often unseen or minor until the disease has progressed, this cancer is often referred to as a silent one.
For all types of ovarian cancer, the five-year survival rate is 45 per cent, according to the American Cancer Society. Women who are diagnosed when they are younger tend to have better prognosis than those older than 65. If ovarian cancer is detected before it has spread outside the ovary, the five-year survival rate is 92 per cent — but only 15 per cent of ovarian cancers are found this early.
For all types of ovarian cancer, the five-year survival rate is 45 per cent.
September is Ovarian Cancer Awareness Month, a time to learn more about the disease and the work being done to fight it. On the first Friday of September, Wear Teal Day, Canadians were asked to wear teal to raise awareness and show solidarity with those living with this disease, and education and fundraising events will be held all around the country this month. See what's happening near you and read on for what you should know about the disease.
What are the types of ovarian cancer?
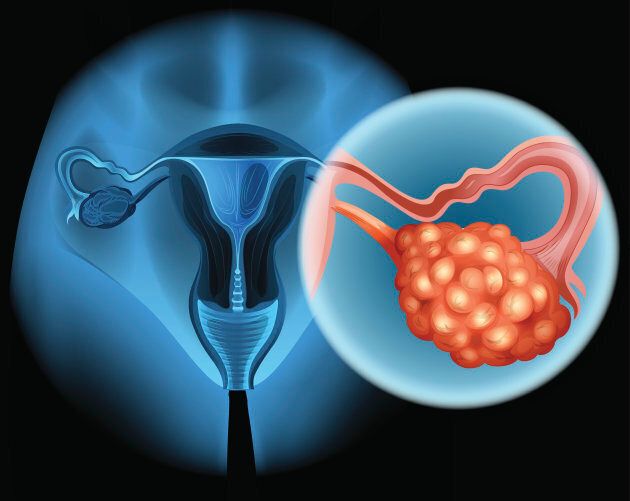
There are three main types of ovarian cancer —epithelial, germ cell, and sex cord stomal — all of which are classified according to the type of cell in which the disease begins, and all of which have different subtypes and characteristics.
There are three main types of ovarian cancer —epithelial, germ cell, and sex cord stomal.
About five to 10 per cent of ovarian cancers are germ cell ovarian cancer, which start from the cells where eggs are formed in the ovaries. These tend to affect women in their 20s and have a few different subtypes. Sex cord stomal cell cancer, which begins in the cells that hold the ovaries together, makes up less than five per cent of ovarian cancer cases in Canada.
What are the risk factors for ovarian cancer?
There is no one set risk factor for ovarian cancer, which can make it difficult to determine one's particular risk profile. "The risk factors for ovarian cancer are a combination of genetic and environmental factors, so completely preventing ovarian cancer will be difficult," says Dr. Sara Cooper, a faculty investigator at HudsonAlpha Institute for Biotechnology.
One project, Information is Power, sequenced 30 genes to determine genetic risk for breast or ovarian cancer and found that half the women with a genetic variant that indicated increased risk of the diseases had no family history of them, she says.
Other risk factors can include age (risk increases as you get older), ethnicity (Ashkenazi Jewish women have higher risk), family history, and reproductive history (risk is higher if you haven't delivered a child).
What is the most common type of ovarian cancer?
Epithelial ovarian cancer makes up nearly 90 per cent of all ovarian cancers, and starts in the cells covering the lining of the fallopian tube or ovary. Clear cell carcinoma is the second most common type of ovarian cancer, and is often associated with endometriosis.
What are the signs and symptoms of ovarian cancer?
The symptoms of ovarian cancer are often vague and non-specific, according to Ovarian Cancer Canada, and can be mistaken for other conditions. They can also often be experienced by people who don't have ovarian cancer.

The common symptoms include persistent bloating and/or increased abdominal size; difficulty eating or feeling full quickly; pain in the pelvic and/or abdominal areas; and urgency or frequency of urination.
Other symptoms can include unexplained weight loss, extreme fatigue, and/or changes in bowel habits. It's important to see your physician if these symptoms are new, persistent, and frequent.
Why is ovarian cancer often diagnosed late?
The primary reason for the often-late diagnosis of ovarian cancer is the lack of symptoms or the fact that many symptoms resemble several other conditions, Cooper says. "In hindsight, women may say they were tired or had some abdominal bloating or pain, but often it is not enough to motivate a doctor's visit," she says.
But there can be may explanations for symptoms like bloating or a sore stomach, most of them non-serious, which can mean they aren't initially recognized as a sign of a serious problem.
In hindsight, women may say they were tired or had some abdominal bloating or pain, but often it is not enough to motivate a doctor's visit.
Another reason why ovarian cancer is often missed until it is in later stages is that we don't have reliable, accessible diagnostic tools to catch it the way we do with cervical cancer and the pap smear, for example.
The only definitive way to diagnose ovarian cancer, to date, is via biopsy, according to Ovarian Cancer Canada. "There is not an accurate blood test, and imaging tests can identify masses but a follow-up biopsy is required to confirm cancer," Cooper says.
"Many masses found in ovaries are benign, so the cost of the imaging test, both in dollars and in stress to the patient is too high to be recommended as a normal screen like what is done for mammography in breast cancer."
How is ovarian cancer treated?
"The standard of care for ovarian cancer treatment is surgical resection combined with cytotoxic chemotherapy," Cooper says. The first line of treatment is usually a platinum chemotherapy, she says, but many tumours become resistant or are resistant to those drugs during treatment, which means additional treatments might be needed and tumours can be difficult to treat.
"Often, a patient's best option if their tumour has proven resistant to therapy is to enroll in one of the many trials around the country," she says.
Can personal risk for ovarian cancer be reduced?
According to Ovarian Cancer Canada, you may be able to lower your personal risk of developing ovarian cancer by using oral contraceptives for five years or longer, by having a full-term pregnancy, and by removing your fallopian tubes during tubal ligation.
Should ovary removal be considered for those at risk?
"In some cases where patients are at extremely high risk, oophorectomy (a surgical procedure to remove one or both of your ovaries) can be considered as a prevention strategy," Cooper says. "The difficult part can be identifying the women who are at such a high risk that a decision would be warranted."

Right now the tests for determining genetic risk are complicated and are not commonly recommended. If you are concerned about your personal risk for ovarian cancer, or have known risk factors that make the disease more likely, speak to your physician. "This is not a decision to be taken lightly as an oophorectomy ends any possibility of future pregnancy and has other significant physical consequences," says Cooper.
Genomics may be the future of treatment
Work is being done right now to improve future treatment options for ovarian cancer. For example, the Cancer Genome Atlas project looks at commonalities and differences in ovarian cancer cells and individuals, and could contribute to personalized medicine that allows for specific treatments for specific individuals based on their tumour type.
How can ovarian cancer be prevented?
"The best prevention is being vigilant about your own health," says Cooper.
The best prevention is being vigilant about your own health.
Talk to your family members to learn if there is any history of ovarian cancer in your family. Advocate for your rights as a patient if you experience symptoms like bloating and stomach pain that don't have an explanation or persist despite treatment. And consider participating in studies and initiatives like Information is Power when you are eligible, both to learn more about your own health and to help further research.
"The best advice I can give is that women should see their gynecologists annually and follow standard screening protocols," she says.
Also on HuffPost: