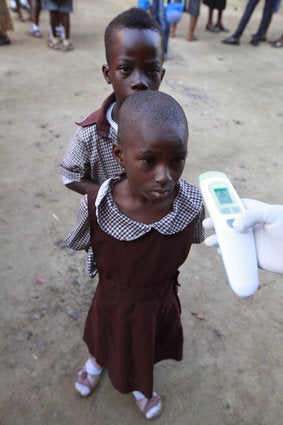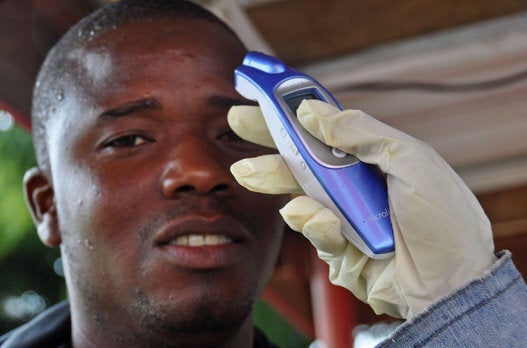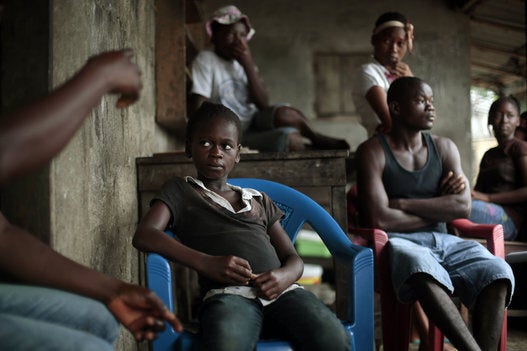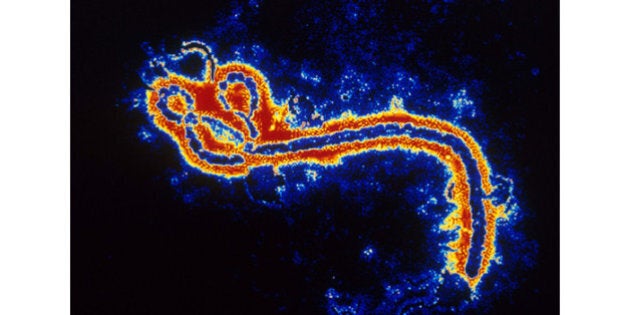
As we all know, here has been one confirmed case of Ebola infection diagnosed in the USA -- Eric Duncan made the news after returning from Liberia and showing those symptoms no one wants. Tragically, Mr. Duncan passed away on Wednesday. Contact tracing indicates that there are an additional 10 persons at "high risk." (In the interest of discouraging any unwarranted panic, do please remember that the virus can only be transmitted via intimate contact with body fluids -- blood, saliva, semen, sweat, etc. -- only after the patient starts showing symptoms, and not during the incubation period.)
In Toronto, meanwhile, ground zero for the SARS scare of 2003, the one suspected case of Ebola turned out to be negative. And a child newly returned from Sierra Leone to Ottawa thankfully also tested negative last month.
So far, Duncan remains the only case of Ebola to have ever been identified outside of Africa.
Earlier, in my Ebola FAQ on my personal blog, I had written that we in the West should not be overly concerned for our own health just yet, not until the first "wild case" appears in North America. Well, I still don't consider Eric Duncan to be a "wild case." He was infected in Liberia, and only diagnosed in North America. I will start to be concerned only when it is shown that someone actually contracted it here in the West.
Why? Because despite some famous failings and constant vulnerabilities of North American public health, one thing we do know how to do well is to contain infectious outbreaks. In fact, it can be argued that much of Western wealth can be linked to a history of well positioned public health investments -- everything from ensuring plentiful clean water to instituting a schedule of mandatory childhood vaccinations. By minimizing the need to respond to expensive population health emergencies, wealthy societies have managed to become wealthier.
Investments in public health are not just important for sustaining individual health and societal prosperity, but also for avoiding security calamity. Disease is recognized as a security threat, and is often modeled along with other human impacts, such as mass migration, as the security dimensions of climate change or natural disasters, worthy of attention from such surprising realms as the Pentagon.
Diseases like Ebola, once discovered, are immediately known to represent an existential threat to resourced populations.Thus, we know that it is in our best interest to invest in containment measures early on. The international response to the current Ebola outbreak is not entirely an act of altruism, then; it is also an act of self-preservation.
We know that identifying and containing infectious diseases is important to all of us. And we know that to do otherwise is to put at risk not only human life, but also societal wealth (which is more important to some people), and indeed societal function itself.
Moreover, we also know how to contain infectious diseases. We know how to do contact tracing, how to set up isolation areas, and how to engage in emergency public education to gain public cooperation in these endeavours.
So why didn't we? Why was the response to Ebola delayed? Allow me to suggest that it has something to do with skewed global priorities still reflecting a neo-colonial sensibility.
The World Health Organization (WHO) was established in the wake of WWII to enact a new vision of global responsibility that flowed from one of the lessons from the war: that wealth and technology were sometimes sufficient to overcome great evils. The WHO's early attempts at Malaria eradication were indicative of this belief, that top-down application of technological solutions (e.g., DDT spraying) were sufficient to defeat one of humanity's oldest intractable foes.
Eradication failed for a number of reasons, one of which was a failure to secure sufficient buy-in and partnership with the beset populations on the ground. In other words, WHO actions were recapitulating the attitudes of the colonial overlords who had only just recently departed the scene. So-called "vertical" Malaria eradication programs were forced to evolve into so-called "horizontal" control programs, which seek to leverage and strengthen existing local assets to achieve a set of health goals that are broader than simple eradication.
It comes as no surprise, then, to learn that many populations in low income countries today view the WHO (and similar organizations) with a suspicion previously reserved for the hated colonials. The WHO, as a result, has retreated to being a self-proclaimed technical body, offering consultation expertise only.
In fact, the WHO Director recently proclaimed, "We are not the first responder ... the government has first priority to take care of their people and provide health care. WHO is a technical agency." And an editorial in Nature responded: if the WHO is not the first responder, then who is?
For the desperately poor countries of West Africa, there are not enough local resources to mount an adequate local response. And, as has already been noted, it is not solely their responsibility; we are all in this together, for more than just touchy-feely reasons.
The CDC, ripe with enthusiasm, resources and expertise, has stepped up to the plate, as has some of the better organized and leveraged NGOs, such as Medecins Sans Frontieres (MSF, or Doctors Without Borders). But action was not taken until the Ebola outbreak had already spread beyond a handful of individuals.
In short, the international community was slow to respond. One reason for this was lack of organization --lack of an obvious first responder, lack of a sensitive governmental trigger process for inviting external aid, lack of an obvious response coordination body, etc.
Another reason was a lack of early warning. And this, really, is key. The ability to rapidly contain an infectious outbreak depends greatly on how early it is identified, and on how early a response can be mobilized. Mobilization was slowed by issues dealing with organizational acumen and political will. Identification, issues, on the other hand are far less nebulous.
It comes down to something population health scientists call "surveillance", a word that alarms the lay public, since it conjures images of Big Brother observing our intimate activities. Epidemiologically, surveillance refers to the practice of being alert to the appearance of disease. Wealthy countries like Canada and the USA maintain scores of simultaneous surveillance systems, both passive and active. They range from a notifiable disease registry, in which clinicians are compelled to report to a central authority all instances of selected diseases, to neighbourhood screening programs.
Our systems are set to detect everything from Tuberculosis to problematic youth behaviours. Many countries have embedded Health Information Systems (HIS), which electronically search linked health databases for signals of possible outbreaks, which are then reported to the proper authorities who organize a deeper investigation and response. No doubt,our systems in the West could benefit from expansion and upgrade. But they are well in advance of comparable systems in the poor countries from where terrifying infectious epidemics originate.
Surveillance systems can be simple or complex. They always cost money. But if they help to identify an outbreak, and thus help to prevent an epidemic, then they save much more money. But poor governments are unlikely to invest in prevention systems when there are immediate health crises that need resources right now: HIV/AIDS, Malaria, maternal and reproductive health issues, etc.
So the Ebola outbreak was not contained early because it was not detected early. And when it was detected, there was an impaired response process. The fault, as I recently heard put quite eloquently by Harvard Dean of Public Health Julio Frenk, is our "failure to invest in global public goods. "
What global public goods? Surveillance systems, international response protocols, and maybe even diagnostic laboratories. The high false-negative rate of some of the field Ebola tests required rapid confirmation from more advanced labs. In Africa, where such labs are not well distributed, this presents a barrier to timely identification and action.
So why haven't these obvious investments been made? Surveillance systems and labs are not without cost. But they do not approach the financial burden of flying emergency isolation and containment teams to Africa. Nor do they compare to the flagrant financial abuses we commit in the name of global security.
A single predator drone, for example, costs more than $4 million. For that same price, an African nation can have a functional national health information system with the beginnings of largely automated disease surveillance signalling process. For that same price, such a country could be peppered with modern laboratories that could confirm diagnoses of Ebola and a host of other infectious agents, providing a constant injection into that society of both public health value and human resources capacity building.
Why haven't these things been done? It's because our international investment priorities are skewed. A nonsensical global war on terror consumes our industrial and military focus. But the real threat to our sustained prosperity and security is not fanatics with shoe bombs; it's an uncontained pandemic virus, antibiotic resistant bacteria, agricultural blight, climate change and other forces having direct impacts on human health.
Let us learn from the present Ebola outbreak, and re-commit ourselves to those crucial international investments in global public goods. As we now see, failure to do so can lead to catastrophic results.
MORE ON HUFFPOST: