By Ramnath Subbaraman & Madhukar Pai
Tuberculosis (TB) is the leading infectious cause of death globally. In 2015, WHO estimated that there were 10.4 million new TB cases worldwide. Six countries accounted for 60 per cent of the total burden, with India accounting for 27 per cent of the global cases. The WHO highlighted that about 4.3 million TB patients globally are "missed" by health systems annually and remain either untreated or unreported to national governments, which may undermine global efforts to combat TB. India alone has more than one million of these missing TB patients every year.
A study we contributed to, published in the journal PLOS Medicine this week, provides insight into gaps in care where TB patients in India's government program go "missing." The researchers use an analysis called the "cascade of care," which estimates the number of patients who successfully reach each step in diagnosis and treatment required to achieve the ideal patient outcome, which is one-year recurrence-free survival in the case of TB.
The TB community has lagged behind in using the cascade analysis for monitoring programs and setting public health targets.
Over the last decade, the HIV community has very effectively used the cascade of care analysis to identify and plug gaps so that more patients receive effective treatment. UNAIDS recently endorsed an ambitious "90-90-90" global target based on the cascade. The TB community has lagged behind in using the cascade analysis for monitoring programs and setting public health targets. To our knowledge, this study is the first published national TB care cascade.
The study finds that, out of about 1.9 million TB patients who reached government TB diagnostic facilities in India in 2013, only about 1.6 million were successfully diagnosed with TB (figure below). Most of the approximately 300,000 undiagnosed TB patients had either sputum smear-negative or multidrug-resistant TB -- two forms of TB disease that cannot be diagnosed using sputum microscopy, the most common TB test currently used in the government program.
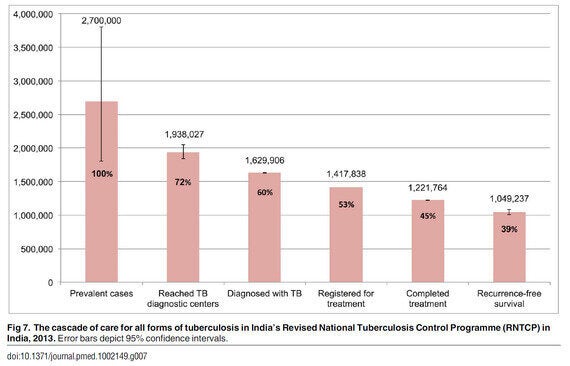
In addition, the study estimates that, out of the 1.6 million diagnosed TB patients, about 1.4 million got started on TB treatment in the government program. About 212,000 patients were successfully diagnosed but did not get started on TB treatment. Previous studies suggest that the government TB program is unable to find some of these diagnosed patients because of poor recordkeeping. Missing phone numbers and addresses and unreadable handwriting in patient registers make it impossible to track some of these patients.
Taken together, these two gaps suggest that about half a million TB patients in India reach government TB diagnostic facilities but are either not successfully diagnosed, or not started on treatment. The study also highlights gaps that occur at the end of the cascade. India's government TB program currently only reports statistics on the number of patients who complete TB treatment; however, the study points out that a considerable percent of these patients will suffer from relapse of TB disease within the first year after completing TB treatment.
What can be done to plug these gaps? Diagnosis of TB patients remains the biggest weakness in the cascade, and this will not change unless India upgrades from testing with sputum microscopy to routine use of rapid molecular tests that have been shown to considerably improve diagnosis of smear-negative and multidrug-resistant TB patients.
While the government has developed an electronic system for notification of TB patients, this needs to be expanded into an electronic medical record system that can be used at the ground level to improve the quality of patient information and help healthcare providers to track TB patients.
Finally, routine one-year follow-up of all TB patients who complete treatment in the government program might help healthcare providers to quickly detect patients who suffer from relapse of TB.
For the first time, this cascade of care study provides an end-to-end view of what happens to TB patients in India as they try to navigate the Indian government's TB program. The government urgently needs to commit considerably greater funds to modernize TB services in India and to track each TB patient, to ensure that all patients make it to the finish line.
India is aware of the need and is starting to address them. Earlier this month, The Lancet published a comment by the Indian Health Minister Mr Jagat Prakash Nadda and Dr. Poonam Khetrapal Singh, head of India's WHO Regional Office for South East Asia. In their Comment, they acknowledged that TB is a bigger problem than imagined in India and other Asian countries, and suggested that TB should be made a top priority on national agendas. They also argued that political commitment should be translated into a comprehensive national TB control plan, and such a plan must be fully funded and implemented promptly by an empowered body that reports to the highest levels of government.
We strongly endorse this plan and hope India's new National Strategic Plan for TB (2017-2023) that is under development will be ambitious, bold, and full funded by the government. That will be a critical investment in India's health and future.
Ramnath Subbaraman is an Associate Physician in the Division of Infectious Diseases, Brigham and Women's Hospital, Boston, MA. He is also an Instructor in Medicine, Harvard Medical School, Boston, MA, and a Research Advisor, Partners for Urban Knowledge, Action, and Research (PUKAR), Mumbai, India
Madhukar Pai is a Canada Research Chair in Epidemiology & Global Health at McGill University, Montreal. He is the Director of McGill Global Health Programs, and the Associate Director of McGill International Tuberculosis Centre. (@paimadhu)
Follow HuffPost Canada Blogs on Facebook
Also on HuffPost: