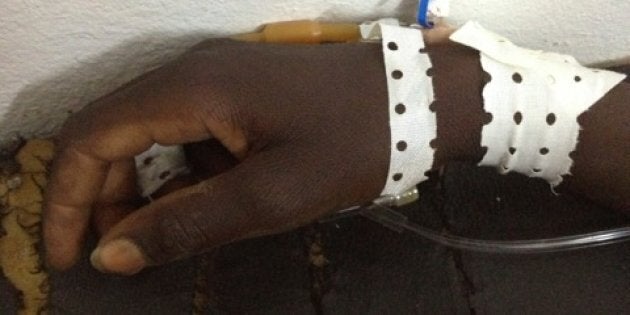
On April 4 late at night, Dr. Guy called me from the hospital. A child had fallen from the roof a house. He asked me to come to the hospital and bring the portable ultrasound machine since he was concerned about a serious abdominal injury.
When I got to the hospital I met Ousmane and his father. The first thing we did was shake hands. Ousmane was 13 years old and was brave and calm. I put my hand on all parts of his abdomen as gently as I could and he winced in pain. Since I graduated from medical school 12 years ago I have come to know that look of pain on a patient's face well. It indicated to me a grave surgical problem. A hole in the right lower quadrant of Ousmane's abdomen indicated a place where a stick or piece of wire had puncture and maybe entered his abdomen. I turned to Guy and told him I was worried. Guy and I agreed this was what we call a "surgical abdomen." I told him we did not need an ultrasound to convince us to take the patient to the operating room.
Nonetheless, I performed the ultrasound of Ousmane's abdomen and it was normal. Very often, in the acute stages of a serious abdominal injury with perforated intestines, the ultrasound is unremarkable. This was a clear case where the physical examination of the patient was a 100 times more useful than technology.
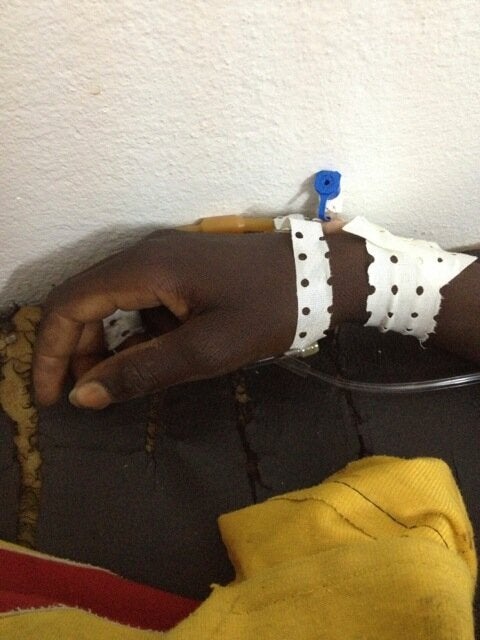
While I prescribed three antibiotics and intravenous fluids for Ousmane, Guy called the surgeon and the surgical team. The MSF car left the hospital in the night, collected all the surgical team and returned. When the surgeon arrived, he took what seemed five seconds to examine Ousmane and agreed on the need for surgery. Within minutes, Ousmane was in the operating theatre. Later yet in the night, Guy informed me our clinical suspicion was correct, the intestines had been perforated. The surgery had gone well.
Ousmane was moved to the intensive care unit. The first days and nights were hard for him. He needed a lot of pain medications. Late at night on April 6 the nurses called me during my overnight on-call duty. They said Ousmane was unwell. I got out of bed and changed quickly into pants and a shirt and took a Land Cruiser to the hospital. The night air coming in the window was hot. The dirt streets were empty. The dust and darkness made it seem like we were driving in fog. It was calm and peaceful. The driver and I drove in silence.
I got to the hospital and examined Ousmane. He was delirious and nauseated. His father shared the bed with him and I could see he tended to him as best he could. I talked to the nurses while I examined Ousmane. Then I prescribed medications for nausea and talked to Ousmane's father through the help of the nursing staff. Ousmane was having a rocky post-operative course.
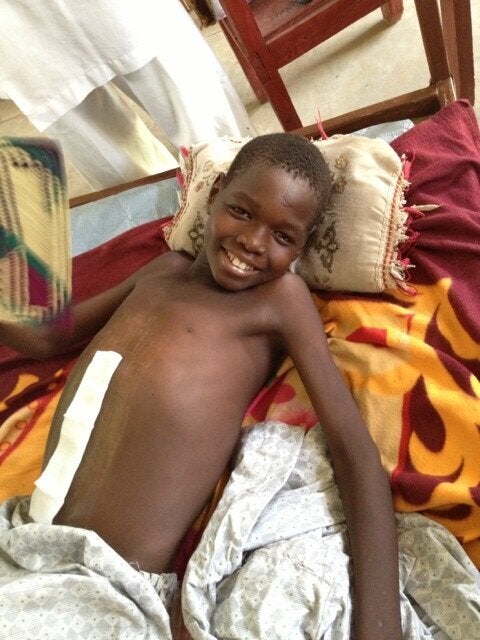
With other doctors on the team taking care of him, and with many things going on in my daily non-clinical work, I honestly somehow forgot about Ousmane in the subsequent days. But on April 13, I was quickly walking through the pediatrics ward and was stunned to see a young boy with a huge smile from ear to ear. It was Ousmane. He was about to go home that very moment, and he had completely recovered. He was a lovely young man. I asked him and his family's permission to take their photos and Ousmane did great taking his own photo with my iphone.

As a medical team leader, I don't work as much in the hospital at night compared to the rest of the medical team of nurses, midwives and doctors. These men and women work long and hard. In some cases, expatriate medics are needing to work seven days a week in the hospital. It's hard and wears you down. My own time is heavily spent on medical strategy, coordinating our efforts with the Ministry of Health and other actors, and doing the behind the scenes work that is crucial to ensure a hospital and outreach team can do their job. I'll be honest with you, that I prefer the bedside medical care -- in the day and in the night.
It is possible to think of MSF's medical work like a scalpel, which we use during surgery. The sharp end is at the bedside with patients and families. It's the crucial end -- and nothing can replace it. But behind the blade is its attachment and then the handle from which to hold the blade. These parts are crucial too. I prefer being at the sharp end -- but I know the attachment and handle is just as important. You can do much with just the blade.
Behind able to go to the hospital at night requires a proverbial blade, its attachment and a handle.
Practically speaking we need drivers, cars, petrol, guards and radio operators to make it happen. We need nurses on duty, who first discover something is wrong. We need logisticians who ensure there are generators to give light to the hospital at night. We need non-medical team members to also order key medications that I or other medics might prescribe at night. We need a coordination team in the capital to reach an agreement with the Ministry of Health that we can work here in Amtiman. And we need donors and supporters who generously give to make all of this possible.
Late at night we need a doctor. But we need a lot more too.
Farewell for now from the house-call....to Chad.
Raghu
Please note: patient names are changed to protect patient identity. All photos are posted with family consent.