"I won't accept new patients if Bill 87 passes. I can't take the risk," a colleague said.
"I don't know how to examine patients if Bill 87 passes," another added.
"I will leave medicine if Bill 87 passes. I can't be a good doctor if I'm scared of patients," a third stated softly.
It's tempting to dismiss these physicians as paranoid, but I wonder, are they the canaries in a coal mine?

I want to work, blissfully ignorant of politics. But with each year that passes, more and more laws are passed at Queen's Park, many of which make no sense, many that are out of touch with reality -- and many that are changing medicine in fundamentally screwed up ways.
I don't understand what the Liberal government is doing to Ontario's health care.
Let's look at Bill 87, the Protecting Patients Act. Its intent sounds good: the government is cracking down on health-care workers who sexually abuse patients.
But Bill 87 is extreme, breeding a culture of fear. It won't just punish the guilty. It will punish anyone suspected of wrongdoing: public shaming, heavy fines and a suspended license, all before guilt is established.
Innocent until proven guilty should be a basic right. The government is targeting healthcare professionals right now -- doctors, nurses, dentists, chiropractors, psychologists and so on. Who's next?
How do I reconcile my duty to patients with the all-too-human need to protect myself?
So I'm upset. I'm furious with the health-care professionals who sexually abused patients and started this mess. But I'm also angry with the Liberal government's scorched-earth response. Two wrongs do not make a right.
Why can't the Liberals simply punish those found guilty? Why must they smear all health-care professionals with the same black brush?
Bill 87 will make ordinary physicians afraid. Any clinical exam, any touch can be interpreted as sexual abuse. Tell me: how will I examine a breast lump? A groin hernia? A heart murmur? Check for rectal cancer? Skin cancer? Scoliosis? How will doctors and midwives deliver babies? How will surgeons remove breast cancers or fix groin hernias? How will nurses put in urinary catheters?
I cannot do my job without examining patients. So how do I reconcile my duty to patients with the all-too-human need to protect myself?
Last week, a patient, suffering from depression wept in my office. Usually I touch their arm in comfort. This time, I hesitated. A simple gesture of support suddenly represented danger and risk. What if the patient mistook my intentions?
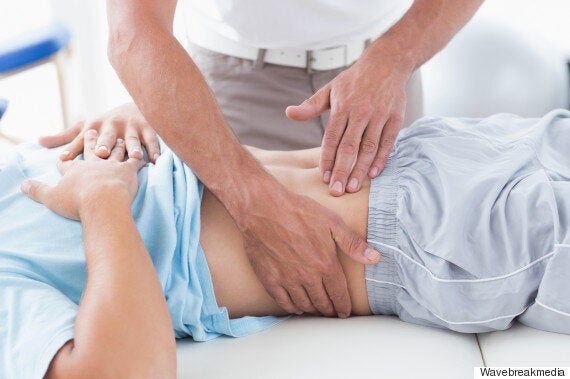
A culture of fear means humanity -- that messy, empathetic, impulsive, compassionate core of humanity -- is tabooed right out of medicine.
Look, I get along just fine with most patients -- but not all. Every doctor and nurse has had a patient misunderstand and cross boundaries. Patients have flirted, yelled, even slammed doors on me. Some physicians have had worse: threats, intimidation, stalking -- truly frightening behaviour. So I worry that some of the most at-risk patients -- the ones with personality disorders, mental illness, addictions and so on -- will be deemed "too risky" and be further marginalized. I hate saying it, but I'm trying to be honest.
Under Bill 87, one patient can ruin my name. They can threaten my license and the livelihood that supports my children, my parents, my secretaries and office staff. That one person could threaten the care of hundreds of other patients relying on me.
Already, hospital administrators are recommending nurse chaperones for every patient encounter. As a family doctor paying $100,000 to $150,000 in overhead costs, the added cost of a nurse chaperone is an impossible expense. Some will close up shop. Some will replace physical exams with tests and imaging, driving up the cost of health care -- but what about the clinical exams that cannot be replaced? Many doctors will document each encounter in minute detail. But at a time when one hour of patient care generates one hour of paperwork, this added burden will have consequences: less time for patients, less accessibility, more burnout.
From a patient perspective, having a third body in the room will change the dynamics. How many more will now hesitate to bring up intimate partner violence? Childhood abuse? STDs? Mental illness? Poverty?
The Liberals have a choice: create laws that make sense and move health care forward - or rubber stamp bad ideas.
I'm trying to understand, but the details don't add up.
Bill 87 takes this culture of fear one step further. It will allow the government unfettered access to personal medical records for all health professionals. Why? "To determine whether the College is fulfilling its duties." I have no idea how personal health records for doctors, nurses, chiropractors, massage therapists, physiotherapists and so on determine the performance of regulatory Colleges. It makes absolutely no sense.
The government has no right to access patient medical records; just because I'm a doctor does not mean they get to peek at mine. Doctors are patients, too.
Last week, a family doctor told me about two suicides out of her medical school class of 100 in the span of one year. Physicians have higher rates of suicide than most. Dr. Shelly Dev wrote that medicine has "emotional weight." Journalist Sharon Kirkey wrote that "doctors are notoriously bad at seeking help, because to declare any kind of mental illness... can be seen as a sign of weakness. Others fear risking their license, their hospital privileges or professional lives."
This fear is about to become reality. A sick doctor cannot care for sick patients.
So I'm asking: how will this protect patients?
Bill 87 has not yet passed. The Liberals have a choice: create laws that make sense and move health care forward -- or rubber stamp bad ideas. If Bill 87 passes unchanged, its intrusive, scorched-earth philosophy will create a paralyzing culture of fear in medicine. A government that OKs a policy like that is not fit to serve.
Follow HuffPost Canada Blogs on Facebook
Also on HuffPost: