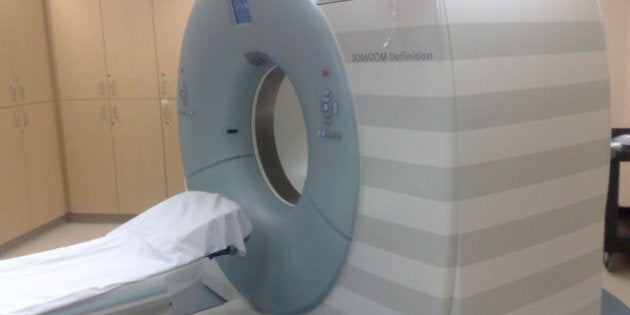
Back in November, before starting my chemo for breast cancer, I had some scans to get a better idea of what was going on in other parts of my body. The hope being, of course, that nothing was going on. Just regular healthy human stuff.
Everything appeared to be okay, except a few small spots lit up on my lungs. Many strange things can take place in the average human body, but when you have cancer, everything gets extra attention and is slightly more suspicious. We weren't sure what these "nodules" were and it is not such a simple task to simply remove them, when you're dealing with an area like the lungs. So the plan was to leave them, do chemo, wait a few months until the chemo had left my body, and do a re-scan to see if there had been any change in size or quantity.
I was not happy that these spots showed up. But I quickly fell into my chemo/cancer routine and was so overwhelmed with everything and feeling so terrible, that my lungs moved to the back of my mind (not literally... obviously that is impossible. I think.). Then chemo came and went, radiation began, and I saw that my dreaded follow-up scan appeared in my hospital schedule.
There is something cancer patients refer to as scanxiety, which, I'm sure you can guess, is having anxiety about upcoming scans and results. Over the past several weeks, I have been suffering from a major case of scanxiety. I have gone through all the scenarios in my head. I have imagined getting the results, hearing my cancer has spread, hearing I have 1-2 years left to live if I'm lucky. I've imagined being thrown back into chemo and never feeling good again for the remainder of whatever time I have left. I thought about how I would tell everyone, and how I would be destroying the happiness of so many loved ones in my life.
Because of this scanxiety, I've felt like my life has been on hold, mentally. I have tried to stop myself from getting excited about any future plans on the horizon. I have been unwilling to let anyone plan any kind of party or celebration for me, as I feared that soon enough, I would be mourning and not celebrating. I have tried to take an interest in everything going on around me and everyone's daily lives and problems, when inside, I have constantly been panicked that I am getting closer and closer to the date when I'm going to be told my life, as I know it, is over.
Thursday, at long last, the day arrived and I had my dreaded CT scan, in the early hours of the morning. Afterwards, I wondered if this would be the last "good" day I'd have. The last day of my former cancer life. I thought maybe I should do something special, in case it was. But I didn't. I just carried on with my normal life and normal day. I got groceries. I watched some TV. I went to bed. I said a prayer to whoever might be listening. Please don't let me die. Not just yet. Thanks.
Today after completing my Herceptin infusion and radiation treatment, I went home. A couple hours later, I received a phone call from my oncologist, who knew I was anxious about my CT scan.
"The areas on your lungs look exactly the same as the first scan. Nothing has changed. If they were cancer, I believe the chemo would have made them disappear. They are exactly the same. Most likely something that has been there since your childhood."
So there you have it. No cancer in my lungs. At least not right now. I am not going to die. At least not today.
After I hung up the phone, I started dancing and jumping around. Then I fell into my chair and burst into tears, everything that I had been trying to bury deep down inside suddenly pouring out of me.
It is hard to describe how I'm feeling right now. You really can't understand until you've walked the walk of cancer and scans and all that jazz. Living life every day, thinking you're about to be told your illness has become incurable... that is some pretty crazy stuff for a young woman to have to think about. For anyone, I suppose. I feel like the heaviest weight imagineable has been lifted off my shoulders. I feel as though I could just float away, in a sea of relief.
For the first time since I was diagnosed, I am choosing to believe that my life could be good again. That I could have years ahead of me. I don't believe this is a definite. I'm not at that point yet, and don't know if I ever will be. But I believe it is a possiblity, and that is enough for me right now. The possibility of life. How exciting.
In one month, I will be on a beach in Jamaica with my husband. We booked the trip last year, and then had to cancel after my diagnosis, a couple months before we were scheduled to go. We re-booked it as a post-radiation/post-chemo trip, in hopes that I would be okay at that point.
That we could celebrate and take a much-needed and much-deserved break from the daily realities we have been facing for almost a year. And now it looks as though it is actually going to happen this time. In one month, I will be okay, and I will be alive. I am going to go to Jamaica and I am going to swim in the Carribean sea and I am going to be grateful for every single second that I am there.
I truly believe that no one on Earth is happier than I am right now at this moment. No one.
And all it took was a bit of cancer. Fancy that.
This post originally appeared on Stephanie's blog at www.passmeanothercupcake.com
