
OTTAWA — Canada is planning for what’s poised to be its largest-ever vaccination campaign.
In a few weeks, the Public Health Agency of Canada (PHAC) is expected to release an interim statement listing which priority groups should get first access to an authorized COVID-19 vaccine, when one or many become available.
Dr. Caroline Quach-Thanh is the chair of the National Advisory Committee on Immunization (NACI), the external advisory group responsible for identifying which groups should get COVID-19 vaccine priority. This sort of triage is necessary and similar to how the H1N1 vaccine was first rolled out.
“Of course the problem currently is we don’t know which vaccine is going to be available and how many doses,” Quach-Thanh told HuffPost Canada.
There won’t be enough vaccines available for everyone, at least at first. The number of doses in that initial stock, which could vary from tens of thousands to millions, will dictate the scale of an initial vaccination campaign.
“We have to remain quite theoretical about it,” Quach-Thanh said.
Watch: Chief public health officer says Health Canada aims to speed COVID-19 vaccine approvals. Story continues below video.
During the H1N1 influenza pandemic, six groups were given priority to the first round of vaccines. They included: people under 65 with chronic medical conditions, pregnant women, children between the ages of six months and five, residents in remote and isolated communities, front-line health-care workers, and household contacts and caregivers of high-risk people and individuals who can’t be vaccinated.
Quach-Thanh said priority groups for early COVID-19 vaccine distribution “might differ a bit because we are now looking at it through a different lens.” But a risk group is still a risk group, she said.
NACI has already identified priority groups for a potential COVID-19 vaccine. That list is currently before provincial and territorial governments, and public health groups for review. Quach-Thanh said notes will be collected and returned to NACI’s committee of experts for final approval before it’s signed off by PHAC for public release.
The interim list of priority groups will be subject to an additional final revision when duration of immunity and the number of available doses of an approved vaccine are known.
“You really have to plan ahead.”
- Dr. Caroline Quach-Thanh, chair of the National Advisory Committee on Immunization
“We have to start thinking about this because if we wait to know what vaccine has made it through to Health Canada, we won’t have enough time to think it through,” the infectious diseases expert told HuffPost Canada. “You really have to plan ahead.”
Because of the pandemic circumstance, Canadians will not have to pay for a COVID-19 vaccine. Quach-Thanh offered a pragmatic explanation: “Because there won’t be enough vaccines for people to purchase it on their own.”
Health care is a provincial and territorial responsibility, so it will be up to those jurisdictions to implement rules and administer vaccine clinics — which could lead to varying approaches like the different school reopening plans across the country. Some provinces and territories, such as British Columbia, Ontario, Manitoba, Quebec, already have living plans in place to mitigate future influenza pandemics.
The process to ensure those plans are scalable and flexible enough to shape future COVID-19 vaccine distribution has many experts looking to the lessons from 2009-2010 when the H1N1 influenza pandemic gripped people’s attention.
“There are so many variables in the current set up because it’s a novel virus,” explained Ian Culbert, executive director of the Canadian Public Health Association. “And that’s what differentiates it so greatly from H1N1.”
* * *
In the spring and summer of 2009, the H1N1 influenza virus was the first flu pandemic the world had seen in 40 years. In Canada, the first cases were recorded in late April. It infected thousands, nearly doubling the number of hospitalized adults between 20 and 64 compared to the seasonal flu. Children under five were also hospitalized at a high rate due to the H1N1 virus. By the pandemic’s end, 428 people had died here. COVID-19, in comparison, has had a more devastating impact, resulting in more than 9,140 deaths and more than 131,000 reported cases as of Friday.
According to Chief Public Health Officer Theresa Tam, 88.5 per cent of people who have reported COVID-19 cases have recovered.

A vaccine for H1N1 was distributed quickly in Canada because the federal government had a contract in place with a domestic supplier to ensure enough vaccine would be available to all Canadians, according to PHAC’s “Lessons Learned” report from the pandemic. Canada ordered 50 million doses of H1N1 vaccine then. And according to Statistics Canada, an estimated 41 per cent of Canadians over the age of 12 were vaccinated in the pandemic then — one of the highest rates in the world.
That vaccination campaign, Canada’s largest up to that date, yields lessons for today.
Batches of vaccine were delivered to provinces and territories as they became available. The unprecedented time called for unprecedented measures.
“Provinces and territories were allowed to stock the vaccine in their centres before it was approved for use, an unusual practice since distribution is normally not allowed until the product is approved for sale,” according to the “Lessons Learned” report. “This was done to reduce the time lag due to the repackaging necessary for shipping smaller quantities of vaccine to smaller centres.”
Health Canada approved a vaccine for H1N1 around the same time the country entered the second wave of the pandemic in mid-October 2009. The federal public health agency declared the pandemic over on Jan. 27, 2010.
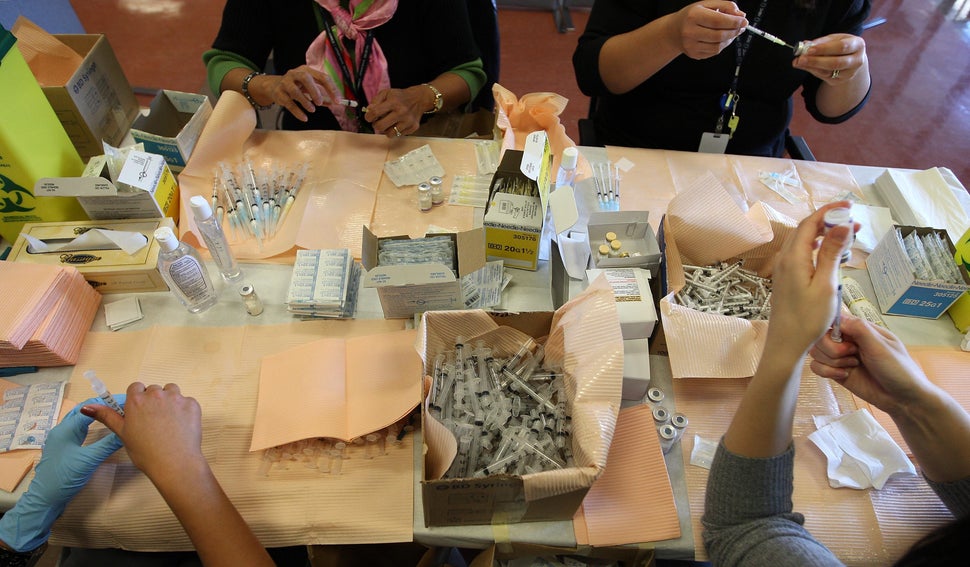
During the vaccination campaign, confusion arose with five vaccines that were available during the immunization period. They included three different H1N1 vaccines and two seasonal influenza vaccines. Public health officials found the range of options “complicated the process in terms of volume of documentation required, staff education and stockpiles.”
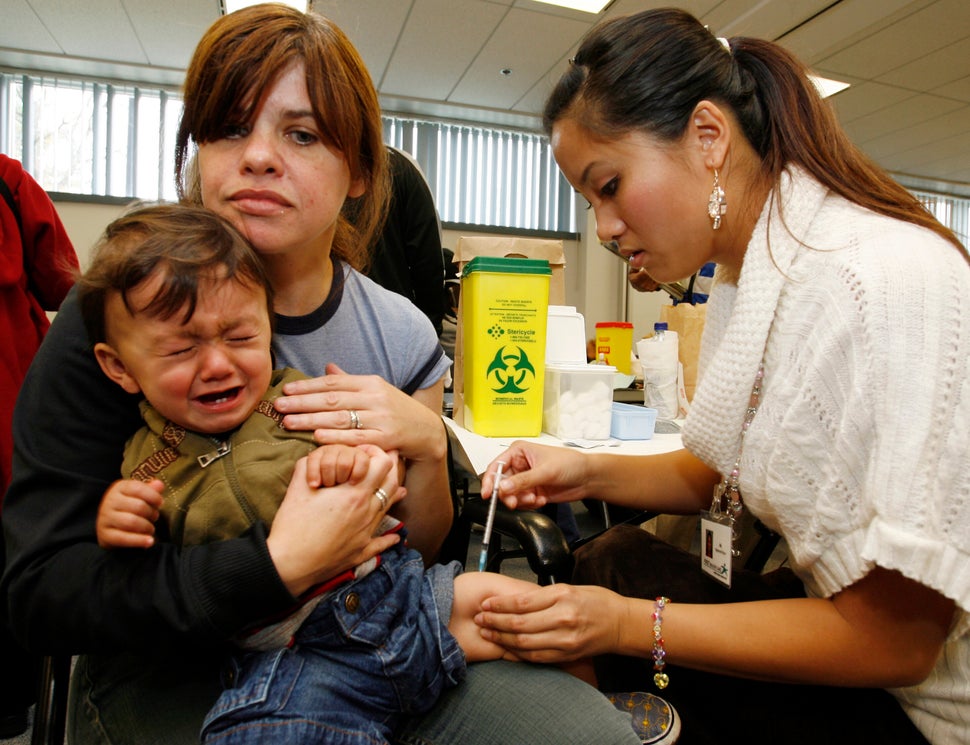
Priority groups crowded H1N1 vaccination clinics, creating long lineups, some that started hours before sunrise. It’s a stark comparison to today when unmasked strangers standing in each other’s two-metre bubbles would be cause for public alarm. Looking at those old images through a new COVID-19 pandemic lens is nothing short of cringe-inducing.
That situation, the risk of creating potential super-spreading events at clinics, is exactly what health officials want to avoid to reduce potential COVID-19 transmissions.
“We look back on pictures of the vaccination clinics for H1N1 and you had hundreds of people in these small, enclosed spaces, no one’s wearing masks or anything else,” Culbert said. “It would look very different for a COVID-19 vaccination clinic.”

To respect physical-distancing measures, COVID-19 vaccination clinics may look to scheduling time slots or having clinics set up in locations where people are working, reducing transmission risk by limiting the need for additional travel.
“I could imagine instead of these mass vaccination clinics where there’s one clinic for a large population, there may be a larger number of smaller clinics so that you don’t have these large crowds gathering, especially indoors,” Culbert told HuffPost.
Flexible early morning and evening hours are also another way to accommodate people who can’t get time off work to get vaccinated. The season when an approved vaccine arrives and what point in the evolution of the pandemic we’ll be in then will also determine how distribution sites are organized.
“Depending on timing, if it’s nicer weather by the time a vaccine comes out, then you could have tents, like open tents, where people could line up and to get a vaccine so that they’re not congregating in an enclosed space,” Culbert said.
Natural and vaccine-developed immunity and how long it lasts is another important factor in designing this massive vaccination program.

Deputy Chief Public Health Officer Howard Njoo said in July that studies have shown for people who have been infected with COVID-19, their natural immunity to the virus doesn’t last long, ranging from a few weeks to several months. Reaching herd immunity by natural infection is “not something that we can count on,” Njoo said.
Waning immunity means increased risk of re-infection. With no one strong vaccine candidate on the immediate horizon, and with only early data to work with, Culbert said it’s currently within the realm of possibility that a viable COVID-19 vaccine “becomes an annual thing just like seasonal influenza.”
At least 88 million COVID-19 vaccine doses guaranteed
The federal government has so far signed four contracts to secure at least 88 million doses of potential COVID-19 vaccines. An additional 102 million doses will be available “at Canada’s discretion,” Public Service and Procurement Minister Anita Anand told reporters Monday.
With Canada’s population at just over 37.5 million, it takes some very quick math to deduce that for full efficacy, some vaccines, if approved, will require more than one dose — and some careful planning now while the world waits for a viable vaccine.
In July, the government initiated a call for tenders on alcohol swabs, bandages, and non-sterile single-use gauze — 75.2 million pieces, each. “We are also procuring supplies that will be needed in the manufacturing and packaging stages of vaccine production in Canada,” Anand said. “When a vaccine is ready, Canada will be ready.”

Health Minister Patty Hajdu has been explicit in saying when a COVID-19 vaccine is made available, it will not be mandatory. “No vaccines are mandatory,” she told reporters at the same press conference.
She said Canadians understand the value of vaccines. “We don’t see the same kind of vaccine hesitancy we see in other countries around the world.” Once a “safe and ethical” vaccine is approved, Hajdu said it will be up to NACI to help identify who and how to vaccinate.
Widespread vaccine uptake is Canada’s best shot at regaining any semblance of pre-pandemic “normalcy,” said Chief Public Health Officer Theresa Tam recently.
Education and outreach need to start now: NACI chair
It’s hard to ignore initial data pointing to seniors in long-term care facilities, new immigrants, and racialized communities as segments of the population at higher risk of being infected with COVID-19. The coronavirus pandemic has renewed attention to systemic barriers in health care that perpetuate inequalities in this country.


While the federal government continues to move and sign deals to secure enough supplies to distribute to the provinces and territories, one of the top concerns for NACI right now is dropping vaccine confidence rates in groups that have been disproportionately impacted by the novel coronavirus.
Quach-Thanh said the top concerns now are about safety, understanding more about potential vaccines’ duration of protection, and implementing a surveillance system to monitor inventory and uptake. There’s a worry at NACI that immigrants and people of colour are less likely to want to be vaccinated.
Government polling suggests a majority of Canadians are open to getting vaccinated when a viable COVID-19 vaccine becomes available. But that number has dropped from 70 per cent in April to 65 per cent in late July. Respondents cited concerns about efficacy and side effects as diminishing factors.
“There’s education and outreach that needs to start now to make sure that we do not miss out on vaccinating the higher-risk population,” Quach-Thanh said.
The circumstances of special populations, such as the homeless, migrant workers, immigrants and refugees who are not fluent in either English or French and rely on friends, family or an association as an intermediary with governments, need to be taken into consideration for vaccine distribution planning.
It’s not because of any genetic predisposition that these people are at elevated risk of being infected with COVID-19, Quach-Thanh said. “But just because of where they work, and living arrangements.”