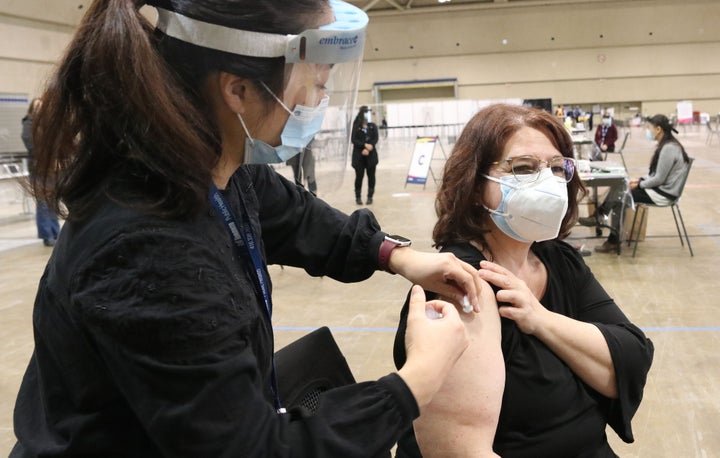
TORONTO — It’s totally normal to have questions about any aspect of your health care. But when it comes to the COVID-19 vaccine, scientists and doctors don’t want the public to turn to random Facebook, Instagram and YouTube accounts for answers. So they’re stepping in.
Krishana Sankar is a doctoral researcher at the University of Toronto’s Faculty of Medicine. She and Tara Moriarty, who directs an infectious diseases research laboratory at the university, have been holding nightly Zoom calls for health-care workers and family members of long-term care residents who have questions about the COVID-19 vaccines.
“It’s OK to have questions, but go to the right places to get your answers,” Sankar told HuffPost Canada. “And then think about it before you share the information.”
“It’s OK to have questions, but go to the right places to get your answers.”
- Krishana Sankar
Their calls have drawn between 30 and 50 participants every night since Jan. 4. One person brought up a false conspiracy theory about the vaccines having microchips in them, but in general, most people just need more information or want to know how to talk to their family members who are nervous about the vaccine, Sankar said.
She shared some of the common questions she’s heard and their answers. Here they are, along with other common questions and answers provided by a panel of doctors with the Ontario Medical Association (OMA).
Which vaccine should you get?
“People should get whichever of the two are offered and available to them,” Sankar said. “Both Pfzer and Moderna vaccines are safe and effective. There are minimal differences between the two and they work in a similar fashion with 95 per cent and 94 per cent efficacy respectively.”
When can you get vaccinated?
This handy calculator can give you an estimate of when you might be eligible for vaccination based on your age, job and a few other factors.
Each province and territory has its own plan for distributing vaccines. In Ontario, vulnerable populations like nursing home residents and health-care workers are first in line. All Ontarians over the age of 60 are expected to start being vaccinated sometime in May, and people younger than that in June or July.
Should you get it if you’re pregnant or breastfeeding?
Sankar said this is one of the common questions they’re hearing.
She said that groups representing gynecologists and obstetricians advise people who are pregnant or breastfeeding to get the vaccine, but says they should make that decision with their doctor.
Ontario had previously said pregnant and breastfeeding people were ineligible for vaccination because these groups weren’t included in clinical trials. But the ministry of health updated its guidance on Jan. 8, saying they “may choose to receive the vaccine after informed counselling and consent.”
Dr. Samantha Hill, a cardiac surgeon and president of the OMA, told reporters Wednesday that she’s breastfeeding and she got the vaccine.
How were the vaccines developed so quickly? Was it rushed?
Dr. Noah Ivers, a family physician at Women’s College Hospital, said at the OMA panel that the vaccines were not rushed even though they were developed “amazingly quickly.”
The scale of the pandemic meant there was unprecedented cooperation between governments and scientists, Dr. Ivers said, and unprecedented financial investment.
“This is a triumph.”
- Dr. Noah Ivers
Clinical trials were able to gather evidence quickly because there was so much spread of COVID-19, he said. In order to find the efficacy of a vaccine, it has to be tested against a control group. So researchers followed people who got the vaccine and compared them to those who didn’t. Since COVID-19 was spreading like mad, the researchers quickly found that people in the control groups were much more likely to get the virus than those who were vaccinated.
This allowed the clinical trials to conclude more quickly than they would for a very rare virus that people in the control group were unlikely to catch.
“This is a triumph,” Dr. Ivers said.
Why are some people worried about the vaccines?
Dr. Sarita Verma, a family physician and dean of the Northern Ontario School of Medicine, said there are three main groups of people who are hesitant to get the vaccine:
- People who know someone or have heard about someone who’s experienced an adverse side effect of a vaccine;
- People from communities that have historically been exploited by the health-care system, including Indigenous people;
- People who have read misinformation online.
She and the other doctors at the OMA panel stressed that adverse side effects are rare.
“The current vaccines that are being used are very safe,” Dr. Upton Allen, head of the Division of Infectious Diseases at SickKids Hospital, said. “Indeed, so far, it appears that they are emerging to be among the safest vaccines in clinical use.”
Doctors will keep meticulous records about everyone who gets the vaccines to detect and study any rare side effects, the doctors said.
“The current vaccines that are being used are very safe.”
- Dr. Upton Allen
Dr. Allen did say that people who take immunosuppressive medication or have had a reaction to polyethylene glycol (PEG) should talk to their doctor before getting vaccinated.
“For most categories of patients, it is fine to proceed with vaccination without discussion with your health-care provider.”
It’s important for doctors and governments to address the specific concerns of Black and Indigenous communities and other people of colour, the doctors at the OMA panel said. Dr. Allen pointed out that many of these groups are the same communities where COVID-19 is taking a disproportionate toll.
There are clear historical reasons why some communities have less trust in the health-care system. Doctors in the 1940s and ’50s gave malnourished children at residential schools experimental treatments and some died or their development was affected, for example. When Inuit were sent south for tuberculosis treatment in the mid-20th century, some families weren’t notified that their relative had died; in other cases, kids returned years later, no longer able to speak their parents’ language.
Dr. Verma shouted out First Nations leaders who are making phone calls and using social media to build trust in the vaccine.
Grand Chief Alvin Fiddler of Nishnawbe Aski Nation, which represents 49 First Nations in Ontario’s Treaty 9 and Treaty 5 territories, shared a photo of his mom getting the vaccine. Eighty-five-year-old Eunice Fiddler volunteered to be the first person at her extended care facility to get the Moderna vaccine.
Grand Chief Fiddler has said it’s important to get people’s consent before they’re given the vaccine, and to provide information about it in the language of their choice, “whether it’s in Ojibway or English or Oji-Cree.”
The last category of “vaccine-hesitant” people are those who’ve read the misinformation that’s rampant online.
Dr. Ivers said people who spew conspiracy theories and misinformation on the internet have been doing it for years, and are one step ahead of doctors. That’s why the OMA held the panel to answer journalists’ questions Wednesday, and Dr. Ivers said he’s working with 19 to Zero to create public information campaigns that are driven by data and respond to what people already believe about vaccines.
Sankar, the researcher organizing question-and-answer Zoom calls, also said she’s working on a national anti-misinformation campaign.
“We do see over time that vaccine confidence and intention is increasing. And I think with coordinated efforts ... we can continue to increase them and head towards herd immunity,” Dr. Ivers said.
“But without that, we will not achieve it. Which means we don’t get back to normal.”
Are you a ‘guinea pig’ if you get it before others?
No.
Clinical trials have been done, Sankar said, and people who are at the front of the line are only there because they’re vulnerable to the virus due to their job, age, health condition or where they live, so they should be protected first.
Dr. Ivers said millions of people around the world have now gotten these vaccines, in addition to the 70,000 people who participated in trials.
“So we actually know quite a lot about the safety of the vaccine. And we know quite a lot about how unsafe it is to get COVID.”
What if you have other questions?
If you have a family doctor, they’re the best person to answer your questions. Dr. Sankar’s other recommended resources are Public Health Ontario and Ottawa Public Health. Dr. Hill suggests AskOntarioDoctors.ca.
Health-care workers and people who live or have a family member living in long-term care can get an invitation to one of Sankar’s question-and-answer calls by emailing tara.moriarty@utoronto.ca.