January would bring good news, Jeremy Taggart had hoped. His 73-year-old mother Beryl would be vaccinated against COVID-19. No longer would he stand in the parking lot of her long-term care home and wave to her through a window for a few moments. Soon, after more than a year apart, he’d walk through Roberta Place’s glass doors and hold her close.
Throughout the fall, Taggart heard politicians and public health officials say vaccines were headed into the arms of Ontario’s most vulnerable residents. He assumed that included Beryl, living with dementia in the Barrie, Ont. home.
But the email Taggart received from Roberta Place on Jan. 8 was not about the vaccine. Instead it signalled the worst of the pandemic was only beginning.
“The spread had started. That’s when I really got scared,” Taggart told HuffPost Canada.

The Simcoe Muskoka District Health Unit had declared an outbreak at the for-profit home after a staff member, who was initially asymptomatic, tested positive during weekly screening. She’d been in close contact with someone who’d travelled internationally.
The virus ripped through Roberta Place like wildfire. Provincial labs later confirmed the outbreak was fuelled by the highly contagious U.K. variant, said Dr. Charles Gardner, the region’s medical officer of health.
Scientists have determined the U.K. variant (named after the country where it was first detected) will likely lead to large increases in cases, hospitalizations and deaths because it is about 56 per cent more transmissible than the original strain. Within 48 hours of declaring the outbreak, cases at Roberta’s Place had ballooned from one to 55. A few days later, three residents died of COVID-19, the next day three more, then two more.
All but two of the 129 residents were infected, as well as three essential visitors, 89 health-care providers and 42 of their family members. Sixty-two people, mostly residents, have died.
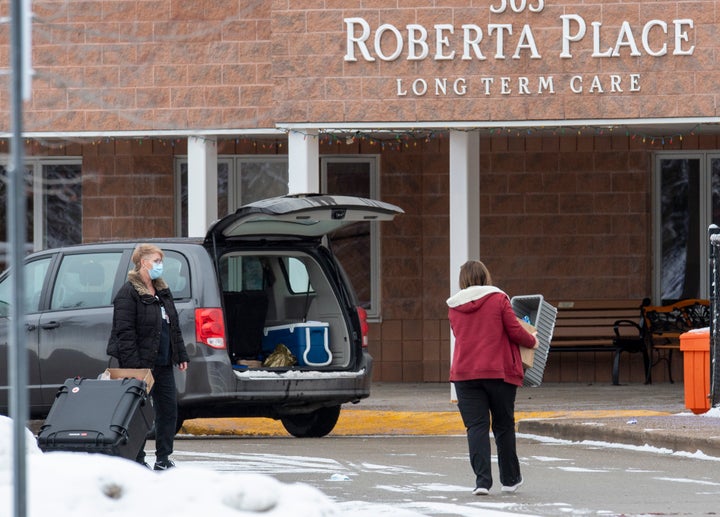
Taggart’s family learned that his mother tested positive for COVID-19 and is currently experiencing fatigue and has lost her appetite, but is stable, he said.
While he’s relieved his mother appears to be doing alright, “you just kind of worry about people who are in worse situations than we are at the moment. A lot of people are battling for their lives.”
Roberta Place is the first known long-term care home in Canada infiltrated by a new strain of COVID-19, one that could already be spreading fast through communities, Gardner warned. Simcoe Muskoka public health has identified two cases in the area not related to Roberta Place.
Gardner called Barrie “ground zero” for the variant.
“If we’re seeing these unanticipated sporadic cases happening, that’s cause for concern,” he said. “There’s potential for a lot of transmission to take place in the city of Barrie and beyond.”
Public health officials connected Simcoe Muskoka region to another case of the variant three-hundred kilometres away in Kingston, Ont. A person travelled to the Barrie area where they contracted the virus from someone with no connection Roberta Place. The person returned to Kingston, where they spread it to four additional people, who have all recovered, confirmed the city’s public health unit.
Roberta Place had one of the worst outbreaks in Ontario due to a confluence of factors, including vaccine rollout challenges, short staffing and a lack of rapid response from the province, experts and critics say.
Firstly, residents and staff had yet to be vaccinated.
In December, Simcoe Muskoka Region received the Pfizer vaccine, but the province directed public health officials there to administer it only at hospitals with access to freezers capable of chilling the vials at the suggested -70 C, said Dr. Colin Lee, associate medical officer of health. That meant many of the region’s most vulnerable seniors were required to wait until the less-fragile Moderna doses arrived.
“I wish I could turn back the clock. If we had a vaccine a month before, I think this outbreak would be a lot less severe.”
- Dr. Colin Lee, Simcoe Muskoka health unit
Lee said officials expected that batch at the beginning of January, before the outbreak at Roberta Place, which they’d send straight to long-term care homes.
“And it was rerouted, as far as I understand, to areas in the province of highest need,” Lee said during a press update. Those places included homes in the Toronto-area and Windsor.
Retired Gen. Rick Hillier, who is overseeing the provincial vaccine roll out, confirmed his team “put the emphasis” on those areas because they were the most threatened.
“If the vaccines moved around that would’ve been why,” Hillier told reporters Monday. “And now we’ve completed that, we’re focused on the rest of Ontario.”
That refocusing came too late for Roberta Place.
It wasn’t until a week after public health officials declared the outbreak that they got permission from the province to use what they had left of the Pfizer vaccine, said Lee.
A mobile vaccine unit administered Pfizer doses to those who were eligible, mostly staff.
“I wish I could turn back the clock,” Lee told reporters last week. “If we had a vaccine a month before, I think this outbreak would be a lot less severe.”

Taggart’s family was told by a doctor that Beryl likely received the vaccine, but by that point she was already infected with the virus. He said the province should’ve vaccinated all long-term care residents in December and is frustrated by delays.
Taggart pointed to the province pausing vaccination efforts for Christmas.
“That’s when they should have been getting their first shot … that would’ve really curbed the spread.”
Long-term care advocate Vivian Stamatopoulos, a professor at Ontario Tech University, said the Roberta Place outbreak demonstrates how the province “dropped the ball” administering vaccines.
“If we had actually treated the vaccination rollout like the emergency it is, we’d have already vaccinated all of long-term care within the first month. It was possible to do that,” she said.
The province said, as of Monday, it has given eligible and willing long-term care residents their first dose in 10 regions, including Simcoe Muskoka.
The home was also short staffed before the outbreak and as workers began falling ill and needing to quarantine, it became a crisis.
The lack of workers caring for residents limited their ability to stop the outbreak, acknowledged David Jarlette, president of Jarlette Health Services, the company that owns Roberta Place.
“The virus came into the home so quickly. We found ourselves not able to have the staffing resources to cohort in a quick and timely fashion,” he said during a press briefing last week.
A provincial inspector conducted a tour of Roberta Place the first week of the outbreak on Jan. 12 to 13 and found Jarlette Health Services “had failed to ensure that the home was a safe and secure environment for residents,” according to the report. Residents with and without COVID-19 were sharing rooms and came into close contact with one another.
Some residents with COVID-19 were out of their rooms, touching surfaces and refusing to stay in isolation, the inspector found.
The union representing Roberta Place workers said staff followed all the right protocols leading up to the outbreak and despite being tired, exhausted and afraid, they continue to work long hours. Some are living away from their families in hotels to try to contain the spread of the variant.
“I’ll be honest, our primary task right now is not in finding blame, it’s in dealing with this inferno. They’re holding back what is akin to a raging fire. They know that if they get it wrong, people’s lives are at stake,” said Ian DeWaard, provincial director of CLAC.
“They know that community spread is possible. Their attention is focused on caring for residents and keeping things contained.”
However, more than 200 doctors and researchers, including Stamatopoulos, say short staffing is a systemic problem that the province needs to address. They signed a letter this week demanding action, including removing profits from long-term care homes, hiring qualified staff and providing urgent training, ensuring staff are paid fairly and employed full-time, and calling in the military immediately to assist with outbreaks “where staffing has collapsed.”
At Roberta Place, extra help didn’t arrive for a week after the outbreak was declared, when the local hospital took control of the home and extra physicians and the Red Cross were called in.
“I really feel strongly that the military should’ve stepped in right at the beginning and should consider doing that in the event of another outbreak in our area,” said Dr. Kelley Wright, one of the physicians who assisted at Roberta Place.
Wright called families to update them about their parents, sometimes with the worst news.
“I had two patients, a husband and wife in the home, and they both passed and I had to tell a family member they were going to lose both their parents in a week, which was one of the hardest things I’ve had to do in my job,” she said. “We can’t have another tragedy like Roberta Place.”
Premier Doug Ford told reporters last week that when he asked why the military wasn’t sent in, he was told, “we don’t need them.”
Health Minister Christine Elliott added that the Red Cross and hospital support is enough to see Roberta Place through the outbreak.
Watch: Moderna shot key to nursing home vaccinations, says Hillier. Story continues below.
Stamatopoulos rejected this explanation and said the province is not listening to the advice of people working on the front-lines of the pandemic.
“It is always a ridiculous reactionary response when the house is already on fire,” she said.
Joanne Nixon’s father, Cyril, is among the fatalities. The 81-year-old, a double amputee with Alzhimer’s disease, was well cared for at Roberta Place, Nixon said. His death was sudden and heartbreaking and her thoughts go out to the staff there.
“As far as I am concerned, everyone who walks through the doors at any health-care facility, be it a nursing home or hospital, whether they are a psw, or a nurse, doctor, cook cleaner, office staff … they are all amazing people who put their own lives and those of all their loved ones at risk,” Nixon said. “I cannot thank them enough.”
She urged the public to take COVID-19 precautions seriously, especially after experiencing first-hand the devastation caused by the variant.
“If people would realize this maybe they would wash their hands properly and wear their masks and we would be able to prevent anyone else from dying” Nixon said.
Update - Feb. 1, 2020: This story has been updated to reflect additional COVID-19 cases and deaths at Roberta Place.