The first time I held my niece, it confirmed something I had been unsure about for over two decades: I wanted to become a parent. I was 31. The average age of first-time mothers in Canada is about 30. Nothing very out of the ordinary, right?
But, I had medically transitioned years ago. I had been on testosterone injections for seven years and had masculinizing chest surgery. My transition felt complete. Perhaps this is why I could begin to envision myself as a parent — a father.

In theory, I could probably become physically pregnant if I discontinued testosterone, but it wasn’t something I felt very open to — though plenty of incredible men do carry their own children.
Fertility preservation seemed like a good option for me. I was about halfway into a PhD program and didn’t want to take a parental leave. To give myself some more time and options, I decided to freeze my eggs.
I had also just learned that the Ontario Ministry of Health was funding fertility preservation for trans people through the Ontario Fertility Program (OFP). But I had reservations — would my eggs still be “good” after all those years of weekly testosterone injections?
“For some trans people, fertility preservation is an important component of transition-related care.”
I made a visit to my family doctor, who specializes in trans care. She assured me that there is no clear evidence that testosterone negatively impacts egg reserve or egg quality. A recent study seems to confirm this, but more research is needed.
My doctor recommended a few fertility clinics in Toronto that had good reputations for working with LGBTQ people. I was referred to the Mount Sinai Fertility Clinic. I felt hopeful.
I was 31 when I had my initial consultation. By the time my name made it to the top of the list for funded fertility preservation, I was nearly 33.
Cost and coverage are major barriers
For some trans people, fertility preservation is an important component of transition-related care. Psychologist and professor Dr. Damien Riggs believes that fertility preservation is a reproductive right for trans people.
A 2017 survey found that 97 per cent of trans people living in Toronto felt that they should be offered fertility preservation prior to beginning hormone therapy. The same survey found that only three per cent had banked sperm or eggs.
The most common barrier noted: Cost.
Ontarians receive provincially funded fertility preservation, while those who live in Nova Scotia (my home province) are on their own — coverage varies by province. This inconsistent access to care simply isn’t fair.
In regions lacking coverage — virtually everywhere outside Ontario — out-of-pocket expenses for egg retrieval and its associated medications often exceed $10,000. This price tag skyrockets when the procedure needs to be repeated to retrieve the number of eggs statistically likely to result in a live birth.
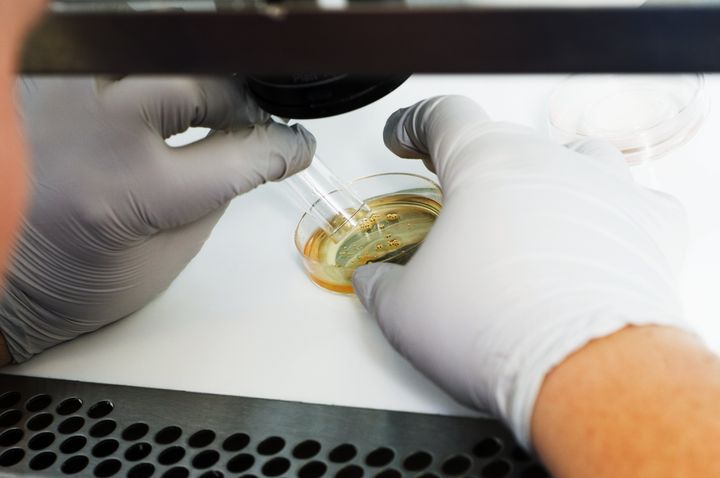
Tax credits are available in Manitoba, New Brunswick and Quebec, but the services must be paid for up front. This constitutes a major financial barrier for the majority of Canadians who would not have a $10,000 (or more) rainy day fertility fund.
On the surface, freezing sperm seems more manageable (under $1,000). But paying storage fees, whether for eggs or sperm, adds up. Yearly storage fees can vary and are not covered by the OFP. I paid $300 in 2018. I paid another $300 in 2019.
These costs are out of reach for the many trans Canadians, who live in poverty due to rampant employment discrimination.
‘Ready for whenever we are’
When I first started transitioning nine years ago, I remember my university health clinic physician encouraging me to think about fertility preservation options. This is considered standard medical practice with trans people who are considering hormone therapy or lower surgeries today.
At the time, delaying starting testosterone by another several months for egg retrieval felt impossible. For trans people beginning medical transition, this can feel like having to choose between fertility or transition.
I’m fortunate that going off testosterone to prepare for egg retrieval was not difficult for me, emotionally, psychologically or otherwise. I knew it would be time-limited, and it was for a worthwhile cause.
However, it’s good practice to assume that discontinuing hormone therapy may be hard for myriad reasons, even when self-motivated by the idea of one day becoming a parent. Health-care providers should be mindful of, and responsive to, this reality, and the many other challenges that LGBTQ people experience with respect to fertility.
“To transmasculine people out there: do not let concerns about testosterone treatment deter you from egg retrieval.”
Once my ovulation cycle resumed, my fertility treatment resembled that of a cisgender female. I began medications that stimulated my ovaries. I also had regular bloodwork and ovarian follicle tracking to see how many follicles were growing.
Many people report symptoms of hormonal mood issues when taking fertility drugs. This was not the case for me. I did have a difficult time with the daily subcutaneous injections into my stomach, however. After years of weekly testosterone injections, I was confident they would be a total breeze. I was wrong.
The actual egg retrieval was the hardest part of the entire experience. I anticipated discomfort — it was agony. I was right to shy away from pregnancy. I was not built for the pain of childbirth! But the procedure was over quickly. Thankfully, my partner was at my side the whole time. Relative to the procedure, the recovery was simple and painless.
Despite seven years of testosterone, the eggs we retrieved went on to produce high-quality embryos. We now have several frozen embryos rated AA, the best possible score, ready for whenever we are.
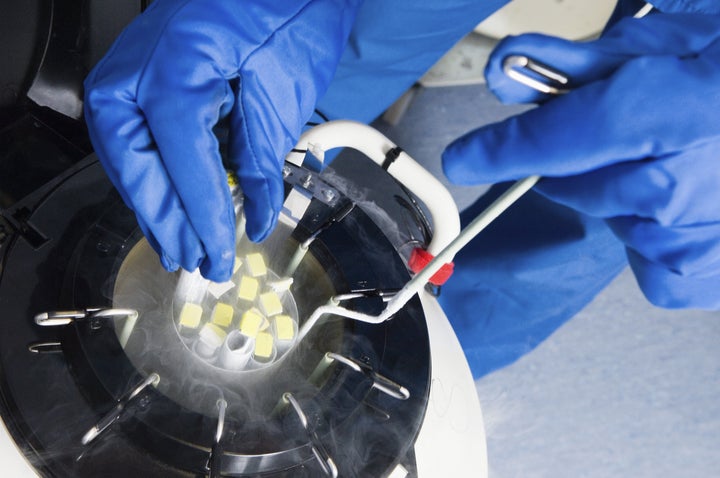
So, to transmasculine people out there: do not let concerns about testosterone treatment deter you from egg retrieval. Age, overall health and genetic factors might be better predictors of egg quality and fertility.
A family — one day
For me, egg retrieval was largely a positive experience. But this didn’t happen through luck alone. It started with Ontario’s policy decision to fund fertility preservation procedures, and continued through to the trans-inclusive medical care I received at my primary care provider and the fertility clinic.
I asked Nurse Practitioner Eileen McMahon, who coordinated all aspects of my fertility care at Mount Sinai, what the clinic did to improve their capacity to work with trans people like me. She told me they had created a trans community advisory committee who made several suggestions. Following the advisory committee’s lead, the clinic provided trans-inclusion training to all staff; revised clinic intake and consent forms; and updated their website and patient handouts to be inclusive of diverse gender identities, bodies, sexualities and relationships.
This is the kind of care and attention that trans people need and deserve in fertility clinics and, more broadly, in all health and social services.
As a patient on the receiving end, I couldn’t help but wonder how things could have turned out differently if I had wound up at a clinic that hadn’t been so sensitive to my needs. If I had been misgendered upon arrival at the clinic, could I have seen the process through to the end? While I don’t have a clear answer, I do feel grateful for the experience that I did have.
After completing egg retrieval and creating embryos, my partner and I now have more options to eventually start a family one day.
Have a personal story you’d like to share on HuffPost Canada? You can find more information here on how to pitch and contact us.
Also on HuffPost: