Content warning: mentions of considering suicide.
I decided to medically transition as a non-binary person at the start of 2020. For me, this looks like weekly at-home low-dose testosterone shots — syringes loaded with a fraction of a teaspoon — that I inject into one of my thighs.
Over the last week, I’ve looked at my half-empty vial with growing dread: Would I have enough to get me through however long the COVID-19 pandemic lasts? Or would the body changes I was looking forward to seeing get shelved indefinitely?
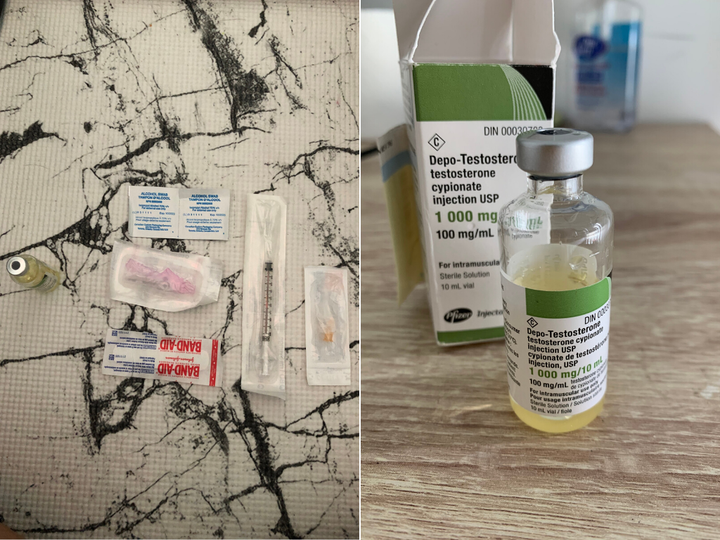
Health-care worries like mine are on the minds of many other trans Canadians. Those waiting for gender-affirming surgeries have received calls from clinics, informing them of cancellations. Life-altering appointments have been cancelled or postponed, as some hospitals limit non-essential visits to prepare for the novel coronavirus overtaking the health-care system. Unease about potential drug shortages has some worried about their access to hormones.
There are mental wellness concerns too; citizens are being urged to stay at home by Prime Minister Justin Trudeau and health authorities, but misgendering from family and community isolation are hazards for many.
That’s not to mention what outcomes a trans Canadian can expect if they test positive for COVID-19.
Existing barriers increase infection risks
Ayden Scheim, an assistant professor at Drexel University, is the co-principal investigator of Trans Pulse Canada, which released the largest health survey of trans Canadians earlier this year.

Scheim says the survey’s findings are relevant to COVID-19, as they show how a pandemic-level crisis could worsen a trans person’s already poor health; half of Trans Pulse’s respondents reported having unmet health needs and 12 per cent who needed urgent care said they avoided going to the ER because they were worried about being treated badly.
“That was obviously really alarming. In a context where people are having COVID-19 symptoms, they need to seek health care. If people are avoiding doing so until their illness has progressed, that’s quite literally life-threatening,” he said.
HuffPost Canada interviewed several Two-Spirit, non-binary, and trans community members living in Canada about their COVID-19 experiences. We also asked health professionals about their concerns. Here’s what they had to say:
Inequities are magnified
As Scheim notes, existing health barriers are even harder to overcome during a pandemic.
“More broadly, we know that trans people face struggles getting competent, respectful care under ideal circumstances. Those inequities are magnified in a crisis situation,” he said. While there’s no data on how Canadians have fared during similar respiratory health crises like the 2003 SARS outbreak, he says the unprecedented pandemic level of COVID-19 means there’s no comparison.
Nour A.* is a trans woman and freelancer. When news about COVID-19 started emerging, she worried she wouldn’t be able to access hormones when the pandemic overloaded Montreal’s health-care system.

She decided to refill her hormones at a walk-in clinic to circumvent health barriers like doctors who are uneducated about trans health nuances. The process took five hours, had her visiting two different clinics, and put Nour in contact with coughing individuals in the waiting room. Once a doctor saw her, it took him three minutes to refill her prescription.
“[City] services are notoriously bad ... that’s something that’s constantly really irritated me. I know what sort of medications I need. I should be able to go to the pharmacy and get what I need,” Nour said. “I can’t live without them.”
Others have struggled to access early refills. Jaden Chattargoon is a Toronto-based trans non-binary community organizer. They were denied a refill by their pharmacist, who said they needed to finish their remaining supply first. To make their current supply last longer, they say they’ve spaced their dose to every two weeks, as opposed to one week.
March 20 was set to be a life milestone for Chattargoon. The social service work student was scheduled to have top surgery in Montreal, an achievement years-in-the-making and funded through community donations.
“All I want is to have freedom from adjusting the way I walk, binding or disguising my chest, [or] feeling deep shame and discomfort,” they said. “My mental health is impacted by the disassociation I experience from time-to-time.”

Gender-affirming surgery confirmations can take years in Canada, a wait that many can’t afford; the mental health toll and risk of suicide or self-harm has been documented among trans Ontarians awaiting their surgery dates. So when COVID-19 was updated to a pandemic, Chattargoon says they entered “panic mode.” Days away from their date, their surgeon assured them the procedure was still good-to-go, but made no promises.
Chattargoon prepared for their Montreal trip, in spite of Facebook comments from cisgender friends that cautioned them against travelling. For Chattargoon, these messages failed to account for how life-saving gender-affirming surgeries are for trans people.
“It was like someone dangled my freedom in front of my face and snatched it away at the last minute,” they said. “I don’t know if it’s happening months from now, or years from now. That’s the part that kills me.”

Hope Adina Adler is a 24-year-old disabled Two-Spirit makeup artist. They have an autoimmune disease called ulcerative colitis, as well as complications-related diagnoses, which have put them in contact with confirmed COVID-19 cases in Ontario hospitals; a long-time friend in Toronto has tested positive for it, too.
They’re happy to hear people are flattening the curve, but aren’t pleased with the racism or flouting of social distancing shown online.
For those who are Indigenous and immunocompromised, Adler recommends prioritizing safety and spiritual needs; they’ve been troubled by the ramifications a pandemic will have on Indigenous communities.
Watch: Trudeau takes questions about Indigenous issues related to COVID-19. Story continues below.
“Smudge sage and cedar and keep yourself hydrated. Wash your hands and try to connect to your spirit during it like meditating,” they said. “We’ve been through worse and we’ll continue to survive and once we make it through this weird time, it’ll be time to continue our work on our rights and for our people to thrive after this.”
No current hormone shortage, but future access is uncertain
Canadian pharmacies are seeing a general increase in customers, but aren’t currently experiencing or anticipating shortages for hormone medication related to COVID-19, according to Health Canada’s database. Those planning to stockpile their prescription drugs may cause unintended shortages, the Canadian Pharmacists Association (CPA) warns.
Scheim notes that he’s heard concerns raised about testosterone supply chains, but echoes CPA’s stance and recommends refills over stockpiles.
However, non-pandemic related hormone shortages aren’t uncommon. Cynthia Leung, a pharmacist with Queen’s Family Health Team in Kingston, Ont. and Canada Drug Shortage member, notes that it isn’t unheard of injectable hormones going out of stock. Much of Canada’s prescription drugs is made in China and India; in the event that commercial supplies dwindle, local pharmacies may not be able to prepare hormones for pick-up.
“Most compounding pharmacies may not have the necessary equipment to compound [hormones]… and not all pharmacies have this capacity,” she wrote over email.
Racism can also be a factor in meeting medical needs. Oji-Cree non-binary trans femme writer jaye simpson notes that Black and Indigenous people have historically been denied safe and affordable health care.
“My health history is rife with mistreatment, from being an Indigenous Youth in Care to now being a fat Indigenous trans woman. I’m often not listened to by ER doctors or staff,” the Vancouver-based writer wrote on Twitter.
Shortages over the last three years forced simpson into periods where medical transitioning was paused. The consequences were body changes that made them feel suicidal.
To avoid repeating those experiences, simpson recently paid $500 out-of-pocket to re-order hormones. Their biggest COVID-19 fear was the risk of medical de-transitioning for Indigenous, Black, and People of Colour who need reliable access to several months of medication.
“Often times this can be misconstrued with hoarding medical supplies, but when it comes to who gets hormones first in this, [it’s the people] with medical access and financial access,” they said.
Gender goes on ‘the backburner’ for some
“Cosplaying a cis person” is how Lee Cumming from Newmarket, Ont. describes their current situation. Cumming, 27, lives with their parents and isn’t out to them as non-binary genderqueer.
“A big part of keeping my sanity is going out to queer spaces,” they said.

Others find that a pandemic has put gender on the backburner. Emerald Lacaille, 29, is a non-binary mental health and housing worker. Being on the frontlines with vulnerable populations means putting aside their identity is a “survival tactic.”
“If I’m not physically OK, how can I be mentally OK?” they ask. “I’m taking care of my mother, I’m taking care of my clients. Gender doesn’t get a minute from me.”
Community care, emotional support more important than ever
While devastated, Chattargoon is keeping their mental health check through chest binding when they need to, keeping busy, workouts, and being optimistic about their situation.
Physical distancing may keep Chattargoon away from IRL get-togethers, but they’ve found support and hope in the virtual queer club scene. As a Club Quarantine regular, they say joining the online dance party filled with queer and trans locals has given them motivation in these times.
“It’s been valuable to stay connected.”
- Mikki Schell
Mikki Schell, a 50-year-old Two-Spirit beadwork artist and self-proclaimed “dissident and matriarch” in Toronto, misses her beading circles, fire-keeping, and socials at the Native Community Centre. She’s taken heart in the check-ins had with Two-Spirit locals who have offered food and supplies.
Online community like caremongering groups have also been a huge asset. Thanks to connections made through social media, Schell has been able to help others do laundry and get help with errands.
“It’s been valuable to stay connected,” she said.
Although it’s hard to know what impact the pandemic will have on trans Canadians’ health care in the long-term, Scheim recommends balancing the need to take precautions with one’s need to protect their mental health.
That may look like continuing to chest bind, but stopping if one starts coughing.
Dr. Karl Neff told Gay Community News that binding shouldn’t put individuals at risk of contacting COVID-19, but those already infected who bind could exacerbate their symptoms.
Others, like Chattargoon and myself, are considering lessening our doses to curb our supply concerns — a measure that Scheim says is OK, as alleviating anxiety is important, too.
Scheim notes that American sources like the Boston Medical Center and the National Center for Transgender Equality have made efforts to inform their patients and keep an open line for them.
He also adds that informal community efforts, such as friends sharing unused medication or supplies with each other, call back to the desperate measures gender-marginalized individuals undertake in lieu of medical professional supervision.
“During health crises and even normal times, there’s a long history of trans people sharing things with each other,” he said. “If people are sharing medication in that context, that’s a pretty reasonable harm reduction approach.”
However, he cautioned against taking undue risks; starting new medications might warrant an ER trip.
*Last name withheld due to concerns over personal safety